You are here: Urology Textbook > Surgery (procedures) > Simple nephrectomy
Open Simple Nephrectomy: Surgical Steps and Complications
Definition
Simple nephrectomy is the surgical removal of a kidney, in contrast to radical nephrectomy, without resection of the adipose capsule, adrenal gland, ureter, or lymph nodes. Alternatives for open nephrectomy are laparoscopic nephrectomy, and retroperitoneoscopic nephrectomy.
Indications for Simple Nephrectomy
- Benign diseases: non-functioning kidney due to benign diseases with symptoms such as hematuria, recurrent urinary tract infections, kidney stones, hydronephrosis, or flank pain.
- Infections: unmanageable sepsis originating from the kidney, renal abscess, emphysematous pyelonephritis.
- Renal trauma
Contraindications
Coagulation disorders. The other contraindications depend on the surgical risk due to the patient's comorbidity, the renal function of the contralateral kidney, and the surgical procedure's impact on the patient's quality of life or life expectancy.
Surgical Technique of Simple Nephrectomy
Preoperative Patient Preparation:
- Perioperative antibiotic prophylaxis if risk factors for surgical site infections are present.
- Perioperative indwelling catheter
- Consider epidural anesthesia
Patient Positioning:
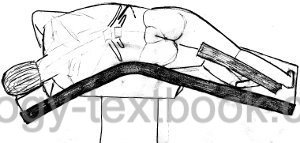 |
Flank Incision:
The simple nephrectomy is usually done via a flank incision. The dissection is done between the 11th and 12th rib to spare the subcostal nerve. Dissect bluntly the layer between the renal fascia and the psoas muscle. Dissect the peritoneum from the ventral portion of the renal fascia until you identify the renal vein. On the right side, mobilize the duodenum from the vena cava (Kocher maneuver).
Dissection of the Renal Hilum:
The ureter is mobilized, dissected, and ligated well below the lower pole of the kidney. The dissection is carried on in the cranial direction following the ureter until the renal hilum is reached. The renal vessels are separated and dissected using overholt clamps and double ligation with Vicryl 0.
Preparation of the Upper Pole:
The kidney is completely detached from the fat capsule and removed, sparing the adrenal gland.
Management of adhesions and scarring:
Especially in benign cases, adhesions between the renal fat and organ capsule are intense and sometimes extend into neighboring organs and vessels (e.g., xanthogranulomatous nephritis, tuberculosis or after multiple kidney surgery). Nephrectomy may be easier in the layer of radical nephrectomy. Alternatively, intracapsular nephrectomy may be performed as a last option: the organ parenchyma is dissected from the organ capsule which remains in the body. This surgical technique is indicated when there is a high risk of adjacent organ injury due to adhesions, such as the removal of a non-functioning kidney transplant.
Drains:
Drainage of the retroperitoneum is often performed, but it is probably unnecessary after uncomplicated nephrectomy.
Postoperative Care after Open Nephrectomy
General Measures:
- Early mobilization
- Intensive respiratory therapy
- Thrombosis prophylaxis
- Laboratory tests (hemoglobin, creatinine)
- Regular physical examination of the abdomen and incision wound.
Analgesia:
Analgesics with a combination of NSAIDs and opioids. Peridural anesthesia facilitates postoperative pain management.
Drains and Catheters:
Quick removal of the bladder catheter after uneventful surgery for stable patients within 1–2 days, wound drainage (often unnecessary) for 1–2 days.
Complications of Open Nephrectomy
- Bleeding and hemorrhage
- Wound infection
- Injury to adjacent organs: liver, spleen (splenectomy), bowel injury, peritonitis, pancreatic tail injury with pancreatic fistula, pneumothorax
- Incisional hernia (due to subcostal nerve injury)
- Chylous fistula due to injury of intestinal lymphatic vessels
| Bowel anastomosis | Index | Radical nephrectomy |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
J. A. Smith, S. S. Howards, G. M. Preminger, and R. R. Dmochowski, Hinman’s Atlas of Urologic Surgery Revised Reprint. Elsevier, 2019.
 Deutsche Version: Technik und Komplikationen der lumbalen Nephrektomie
Deutsche Version: Technik und Komplikationen der lumbalen Nephrektomie
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.