You are here: Urology Textbook > Kidneys > Renal sarcoma
Diagnosis and Treatment of Renal Sarcoma
Renal sarcomas are rare malignant tumors of the kidney derived from mesenchymal cells.
Epidemiology
1–2% of all malignant renal tumors. Peak incidence in the fifth decade of life.
Pathology of Renal Sarcomas
Histology:
Leiomyosarcoma is the most common renal sarcoma, followed by liposarcoma. Less common sarcomas are, e.g., fibrosarcoma, rhabdomyosarcoma, osteosarcoma, malignant fibrous histiocytoma, and angiosarcoma. The pathological distinction between renal sarcoma and sarcomatoid renal cell carcinoma may be difficult.
Origin and growth:
Renal sarcomas typically arise from the organ capsule or the perisinuous space. They grow rapidly to a large size without lymphadenopathy. Due to their origin from mesenchymal cells, renal sarcomas easily cross anatomical boundaries like fascias. Although surrounded by a pseudo-capsule, the tumor may have spread beyond the capsule, explaining the frequent local recurrences after radical surgery.
Metastasis:
High-grade sarcomas metastasize most commonly to the lungs, lymph nodes, and liver.
.Signs and Symptoms of Renal Sarcomas
Renal sarcomas often present with signs of an advanced tumor: flank pain, flank tumor, and hematuria. Tumor growth is fast.
Diagnostic Workup
Abdominal CT:
Large soft tissue mass originating from the kidney [fig. renal sarcoma]. Osteosarcomas show extensive calcifications and liposarcomas contain adipose tissue.
Chest CT:
To complete staging.
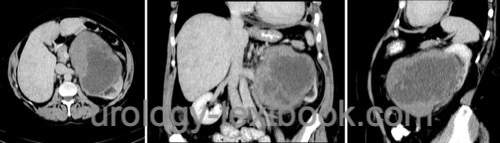 |
Differential Diagnosis
Retroperitoneal sarcoma.
Therapy of Renal Sarcomas
Radical nephrectomy:
Radical nephrectomy with en bloc resection of adjacent organs (e.g., spleen, pancreatic tail, or colon) offers the best chance for cure. Despite maximum resection, local recurrences are common, and repeat resections may be necessary.
Adjuvant radiotherapy and chemotherapy:
Adjuvant therapy is often applied since the prognosis is poor. The benefit of adjuvant therapy is not as well defined as for sarcomas of the extremity. The response rate of chemotherapy for metastatic sarcoma is low.
Prognosis
Renal sarcomas have a poor prognosis compared to sarcomas in other localizations. The grading (differentiation) and margin status after resection are significant prognostic factors. The overall 1-, 3-, and 5-year survival rate was 86%, 41%, and 15% (Wang et al., 2011). The median survival was 28 months. After two years, only 10% were free of disease. The median survival with metastases or after recurrence was 8–10 months.
| Wilms tumor | Index | Renal lymphoma |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Wang, X.; Xu, R.; Yan, L.; Zhuang, J.; Wei, B.; Kang,
D.; Wu, K.; Xie, L.; Xie, Z.; Wei, Q.; Li, X.; Zeng, H. & Lu, Y.
Adult
renal sarcoma: clinical features and survival in a series of patients
treated at a high-volume institution.
Urology 2011, 77, 836-841.
 Deutsche Version: Nierensarkom
Deutsche Version: Nierensarkom
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.