You are here: Urology Textbook > Prostate > Prostate cancer > Definition
Prostate Cancer: Epidemiology and Etiology
- Prostate cancer: Epidemiology and etiology
- Prostate cancer: Pathology
- Prostate cancer: Signs and symptoms
- Prostate cancer: Screening
- Prostate cancer: Staging
- Prostate cancer: Treatment options
- Prostate cancer: Active surveillance
- Prostate cancer: Prostatectomy
- Prostate cancer: Radiation therapy
- Prostate cancer: Brachytherapy
- Prostate cancer: TURP and experimental treatment options
- Prostate cancer: Hormonal therapy of advanced prostate cancer
- Prostate cancer: Treatment of castration-resistant prostate cancer
Guidelines and review literature: (EAU Guidelines Prostate Cancer) (S3-Leitlinie Prostatakarzinom) (Walsh-Campbell Urology).
Definition of Prostate Cancer
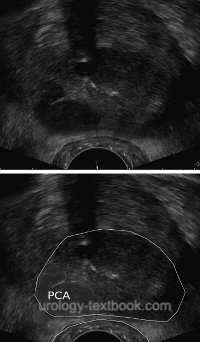
Prostate cancer is a common adenocarcinoma of the prostate with very variable clinical course.
 |
Epidemiology of Prostate Cancer
Prostate cancer is the most common cancer in Germany. It is the third most common cause of cancer death (10%). The incidence in Germany is 100/100000. The mortality is slowly decreasing, with a mortality rate 2018 of about 20-30/100.000 (RKI, 2021).
Age of onset:
The average age at diagnosis is 71.4 years, and the average age for death due to prostate cancer is 78 years. The 5-year survival rate is thus the rule; therefore, 5-year survival rates do not help judge the effectiveness of a treatment option. The diagnosis of "prostate cancer" reduces the 5-year survival rate by 1%, and the 10-year survival rate by 5%, compared to the age group without prostate cancer diagnosis.
Incidence of prostate cancer:
There are great differences between geographical origin and ethnicity: the incidence in the US is between 110 (white Americans) and 170 (black Americans). In Spain, the incidence is 36/100000, and in Sweden, 91/100000. The annual incidence rate increases with age, from about 50/100000 in 60 years old to more than 400/100000 between the ages 75 to 85.
Prevalence of prostate cancer:
The prevalence of prostate cancer amounts to 50–64% in men aged 60–80 years; the data are derived from autopsy studies. The high prevalence also includes a high proportion of small prostate tumors with good differentiation, which are not clinically significant. Approximately 40% of the male population in Germany carry the risk of developing prostate cancer during their lifetime. Only about 10% are symptomatic and only 3% die from prostate cancer; up to 90% of pathologically discoverable carcinomas do not lead to death.
Etiology of Prostate Cancer
Genes are not everything: "Genes load the gun, but lifestyle pulls the trigger", aphorism by Elliott Joslin. Review literature: (DeMarzo et al., 2003).
Genetic Predisposition
Ethnicity:
The different incidences of prostate cancer, depending on ethnic background, suggest a genetic predisposition to prostate carcinoma. The risk for prostate cancer in the United States is highest for black men, followed by white men, and is lowest for Asian men. The prostate cancer risk for Asian men living in the US amounts to 50–100% of the incidence compared to white men, much higher than incidence figures from Asia. The responsible environmental factors have not yet been clearly identified; differences in nutrition are probably the most significant.
Familial prostate cancer:
By definition, familial prostate cancer is present if at least three members are affected by prostate cancer (or at least two members under 55 years). Overall, the proportion of familial prostate cancer is 9%. In contrast, for men with prostate cancer before age 55, 30–40% have familial prostate cancer. Several dominantly inherited genes are thought to be responsible. The risk for prostate cancer is doubled if one first-degree relative is diagnosed with prostate cancer. The risk rises to 5 to 11-fold if several first-degree relatives are diagnosed with prostate cancer (Bratt et al., 2002).
Molecular factors
A combination of different genetic polymorphisms leads (together with a risky lifestyle) to prostate cancer. A variety of molecular changes have been described: activation of PI3/Akt signaling, PTEN/MMAC tumor suppressor gene, epigenetic changes such as DNA methylation, epidermal growth factor receptor (EGFR), telomerase, Glutathione-S-transferase pi, p27 tumor suppressor gene, translocations on chromosome 8q, probably with activation of Myc oncogene, gene deletions on chromosome 8p, p53 tumor suppressor gene, bcl-2, cadherins, IGF-1, changes in the extracellular matrix, increased angiogenesis, MAPK, COX-2, VEGF (vascular endothelial growth factor), and sVCAM-1 (soluble vascular cell adhesion molecule-1).
Chronic inflammation and prostate cancer risk
Chronic prostatitis increases the risk of prostate cancer, explained by the chronic release of cell mediators and the generation of reactive oxygen species. Chronic inflammation and genetic changes (see above) constitute the first androgen-independent steps in the pathogenesis of prostate cancer. Acetylsalicylic acid reduces prostate cancer risk by 30% (relative risk 0.7), but the data are still scanty.
Testosterone and androgen receptor changes
Prostate cancer does not arise in eunuchs and castration results in a significant slowing of advanced disease. However, testosterone is not considered a carcinogen but acts as a promoter in growing tumors. A testosterone concentration in the upper quartile doubles the risk of developing prostate cancer. Several genetic polymorphisms of the androgen receptors increase the risk of prostate cancer.
Environmental factors
The incidence of clinically insignificant prostate cancer is the same worldwide. The increased prostate cancer risk of Asian men who emigrated to the United States proves the influence of environmental factors as a cause of prostate cancer. The best data is available for diet and prostate cancer risk.
Diet:
Many food components are known to increase or decrease the prostate cancer risk (Masko et al., 2013). However, a special diet to avoid prostate cancer is not possible. General health recommendations are helpful, such as normalizing body weight, increasing physical activity, a healthy diet focusing on vegetables, and reducing alcohol consumption.
High-fat food:
Food rich in animal fats increases the risk of developing advanced prostate cancer.
Soy-rich diet:
A soy-rich diet is protective against the development of prostate carcinoma. Responsible isoflavones in soy products are among others genistein, daidzein, and glycetin. Isoflavones are phytoestrogens (Zhang et al., 2016).
Selenium deficiency:
Selenium deficiency is considered a risk factor for prostate cancer. The substitution of selenium has reduced (in some studies) the risk of prostate cancer. The protective effect of selenium is explained by different mechanisms: antioxidant activity, improved immune function, inducing apoptosis, and reduction of cell proliferation. The SELECT study showed no difference in the prevention of prostate cancer.
Diet without seafood:
A diet without seafood can double or triple the risk of prostate cancer.
Beta-carotene deficiency:
Beta-carotene is the precursor of vitamin A. Beta-carotene deficiency increases the risk of prostate cancer (RR 1.3), the substitution with beta-carotene reduced the risk for prostate cancer (RR 0.68).
Vitamin D deficiency:
Vitamin D deficiency may be a risk factor for prostate cancer. The benefits of vitamin D supplementation is controversial.
Tomato products:
A diet rich in tomato products reduces the risk of prostate cancer. Lycopene is an antioxidant in tomato products and is responsible for the decreased risk. In addition, lycopene slows the progression of metastatic prostate cancer.
Smoking:
Smoking is a relevant risk factor of prostate cancer (Kenfield et al., 2011):
- Smoking at the time of prostate cancer diagnosis increases the risk of advanced prostate cancer
- Smoking is a risk factor for a relapse of prostate cancer after primary treatment (38% vs. 26%)
- Smoking is a risk factor for death from prostate cancer (15.3/1000 vs. 9.6/1000 person-years)
Cardiovascular risk factors:
The metabolic syndrome increases the prostate cancer risk.
Alcohol
Alcohol consumption increases the risk of cancer. The data for prostate cancer is inconsistent. In some trials, beer consumption was identified as a risk factor, while other studies found no correlation between alcohol and prostate cancer risk, or even a protective effect of red wine (Downer et al., 2019).
Vasectomy:
No association could be found in a recent meta-analysis (Bhindi et al., 2017). The increased risk after vasectomy in some studies may be explained by a higher prevalence of screening in patients after vasectomy.
Sexuality:
Although some studies showed that a history of sexually transmitted diseases or early beginning of intercourse is a risk factor for prostate cancer (relative risk 2.3), other studies failed to confirm this.
Other environmental factors:
Conflicting and controversial data for pesticides, electromagnetic fields, polychlorinated biphenyls, and dust mite allergy.
| Seminal vesicle cyst | Index | Prostate cancer: pathology |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Bratt 2002 BRATT, O.:
Hereditary prostate cancer: clinical aspects.
In: J Urol
168 (2002), Nr. 3, S. 906–13
N. Mottet (Chair), J. Bellmunt, E. Briers (Patient Representative), R.C.N. van den Bergh (Guidelines Associate), M. Bolla, N.J. van Casteren (Guidelines Associate), P. Cornford, S. Culine, S. Joniau, T. Lam, M.D. Mason, V. Matveev, H. van der Poel, T.H. van der Kwast, O. Rouvière, T. Wiegel Guidelines on Prostate Cancer of the European Association of Urology (EAU), https://uroweb.org/guidelines/prostate-cancer/.
DeMarzo u.a. 2003 DEMARZO, A. M. ; NELSON,
W. G. ; ISAACS, W. B. ; EPSTEIN, J. I.:
Pathological and molecular aspects of prostate cancer.
In: Lancet
361 (2003), Nr. 9361, S. 955–64
Gronberg 2003 GRONBERG, H.:
Prostate cancer epidemiology.
In: Lancet
361 (2003), Nr. 9360, S. 859–64
Kenfield, S. A.; Stampfer, M. J.; Chan, J. M. &
Giovannucci, E.
Smoking and prostate cancer survival and recurrence.
JAMA,
2011, 305, 2548-2555
Masko, E. M.; Allott, E. H. & Freedland, S. J.
The relationship between nutrition and prostate cancer: is more always better?
Eur
Urol, 2013, 63, 810-820.
Wein, A. J.; Kavoussi, L. R.; Partin, A. P. & Peters, C. A.
Campbell-Walsh Urology
. Elsevier, 2015. ISBN 978-1455775675.
Zhang, H.-Y.; Cui, J.; Zhang, Y.; Wang, Z.-L.; Chong,
T. & Wang, Z.-M.
Isoflavones and Prostate Cancer: A Review of Some
Critical Issues.
Chin Med J (Engl), 2016, 129,
341-347
Robert-Koch-Institut Krebs in Deutschland. www.krebsdaten.de
 Deutsche Version: Prostatakarzinom
Deutsche Version: Prostatakarzinom
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.