You are here: Urology Textbook > Kidneys > Simple renal cyst
Renal Cysts: Definitions, Diagnosis and Treatment
Definitions of Renal Cysts
Simple renal cyst
A simple renal cyst is a solitary or multiple, unilateral or bilateral, round, fluid-filled lesion of the kidney without communication with the pyelocalyceal system and without suspicion of malignancy.
Parapelvic renal cyst
A parapelvic renal cyst is a renal cyst located adjacent to the renal pelvis.
Peripelvic sinus cysts:
Usually multiple and often bilateral dilatations of the lymphatic vessels in the renal sinus. Because they lack an epithelial lining, they are not true renal cysts.
Complicated renal cyst
A complicated renal cyst is a cystic renal lesion with at least one atypical feature that does not allow secure classification as benign. Examples include septa, wall thickening, calcifications, hemorrhagic or proteinaceous content, contrast enhancement, or nodular components.
 |
Epidemiology
The prevalence rate of kidney cysts increases with age: 20% at 40 years and 33% at 60 years of age.
Etiology and Pathology of Kidney Cysts
Causes of simple renal cyst:
Simple renal cysts derive from a segment of the nephron. Typical peripelvic sinus cysts probably derive from lymphatic vessels, often associated with nephrolithiasis or urinary obstruction.
Pathology of a simple renal cyst:
Simple renal cysts have a fibrous cyst wall lined with a simple flat to cuboidal epithelium.
Signs and Symptoms
Kidney cysts usually do not cause any symptoms. Simple kidney cysts may cause complications like:
- Abdominal or lumbar pain: due to the displacement of abdominal organs, rupture, or bleeding of the renal cyst.
- Hematuria: due to rupture of a renal cyst into the pyelocalyceal system.
- Arterial hypertension: by compression of the renal artery.
- Hydronephrosis: due to compression of the ureter or renal pelvis.
- Infection: With fever and flank pain.
Diagnosis
Most important with imaging of renal cysts is the classification into simple (benign) or complex (potential malign) renal cysts.
Ultrasound Imaging:
Sonographic criteria for a simple renal cyst are:
- Round lesion of the kidney with echo-free content
- No septa
- No thickening of the round to oval cyst wall, no calcifications
- Posterior acoustic enhancement
- Edge shadowing artifact
If ultrasound findings are atypical, contrast-enhanced CT or MRI is indicated.
Computed Tomography (CT)
CT imaging is indicated for suspicious ultrasound findings such as septation, clustering of cysts, wall thickening or calcification or echogenic contents of the cyst.
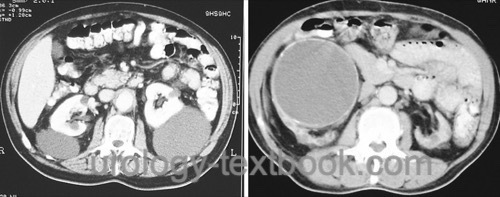
The criteria for a simple renal cyst in computed tomography are similar to the ultrasound (see above); the density is −10 to 20 HU. A simple hyperdense cyst with 20–90 HU is also possible. The most crucial criterion for a benign cyst is no enhancement of the cyst or the cyst wall after infusion of contrast medium. Calcifications are not obligate suspect [fig simple renal cysts].
Bosniak Classification of renal cystic masses (Israel and Bosniak, 2005):
- Bosniak I: clearly benign cyst. No risk of malignancy.
- Bosniak II: few thin (<1 mm) septa or thin calcifications (thickness not measurable), hyperdense lesions (due to proteinaceous or hemorrhagic contents) are non-enhancing after contrast medium infusion, size <3 cm. The risk of malignancy is 0%; follow-up is unnecessary.
- Bosniak IIF: this group subsumes cysts, which cannot be clearly assigned to Bosniak II or III. The risk of malignancy is 5%, and close follow-up is necessary (the 'F' in 2F is for 'follow').
- Bosniak III: not clearly benign cyst: wall or septa with more than 1 mm thickness and measurable enhancement. Surgical excision is necessary, and the risk of malignancy is 50%.
- Bosniak IV: cyst with clear malign criteria; partial nephrectomy or radical nephrectomy is necessary. The risk of malignancy is 75–90%.
Contrast-enhanced ultrasound imaging:
CEUS can improve the diagnostic value of ultrasound imaging (operator-dependent) and may reduce the need for CT for suspicious cysts.
Magnetic Resonance Imaging (MRI)
MRI is a good alternative to computed tomography, especially when follow-up of suspicious lesions is required. MRI avoids the high radiation exposure of a multiphase ct examination and provides higher soft-tissue contrast with better differentiation of hemorrhagic or lipomatous components. Patient cooperation during the examination is important to minimize artifacts caused by respiratory motion of the kidneys.
Treatment of Simple Renal Cysts
Asymptomatic simple renal cysts do not require treatment or routine follow-up. Indications for treatment include symptoms, urinary obstruction, recurrent hemorrhage, infection, or, rarely, or severe hypertension with a plausible causal relationship.
Percutaneous Puncture and Aspiration of Renal Cysts
Pain due to a kidney cyst should disappear after diagnostic puncture and aspiration, at least for a while. A single puncture and aspiration cure a small proportion of patients. Cytology and creatinine measurement in the aspirate are not mandatory for simple renal cysts. If the cyst (and symptoms) recur, definitive treatment is possible with a percutaneous or laparoscopic approach (see below).
Percutaneous Sclerotherapy of Renal Cysts
Percutaneous aspiration followed by sclerotherapy is an established minimally invasive treatment for symptomatic simple renal cysts. A thin nephrostomy tube is placed into the renal cyst with ultrasound guidance. The cyst contents are aspirated and the volume is measured. Instillation of contrast medium confirms the diagnosis; the contrast medium must not opacify the collecting system. Cytology and creatinine measurement in the aspirate are not mandatory for simple renal cysts.
The most commonly used sclerosant is ethanol (99%); the dosage is 20% of the cyst volume to a maximum of 100 ml. The alcohol is left 90–120 min in the cyst: the longer the alcohol contact (several fillings, contact time), the lower the recurrence rate. An alternative sclerosant is polidocanol. A relapse of the cyst occurs in approximately 10–30%. Percutaneous sclerotherapy can be repeated.
Laparoscopic Deroofing of Kidney Cysts
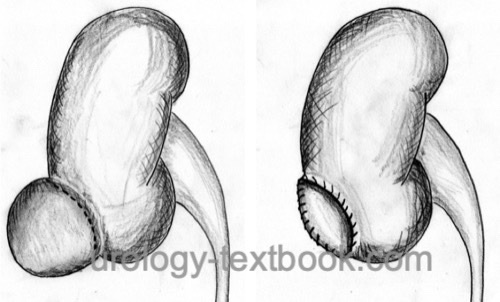
Laparoscopic or retroperitoneoscopic marsupialization is particularly useful for large, recurrent, or unfavorably located symptomatic simple renal cysts. Compared with percutaneous aspiration followed by sclerotherapy, it offers a lower recurrence rate but is more invasive. Laparoscopic or retroperitoneoscopic approach depends on the location and expertise. If the cyst is in anatomic proximity to the ureter, the ureter has to be identified and separated from the cyst wall. The cyst wall is circularly incised near the renal parenchyma (deroofing). The base of the cyst remains in situ. The cyst roof is sent for pathology. Hemostasis is essential and achieved with bipolar cauterization or continuous stitching of the remaining cyst wall. Laparoscopic cyst deroofing is used for very large renal cysts.
 |
Prognosis of Simple Kidney Cysts
Simple renal cysts often show slow growth over years. An increase in size alone does not prove malignancy; morphological features, and in particular newly appearing or increasing complexity according to Bosniak classification, are decisive for risk assessment.
| Multilocular cyst | Index | Parapelvic cysts |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Israel, G. M. & Bosniak, M. A.
An update of the Bosniak renal cyst classification system.
Urology, 2005, 66, 484-488
 Deutsche Version: Nierenzyste
Deutsche Version: Nierenzyste
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.