You are here: Urology Textbook > Bladder > Bacterial cystitis
Etiology and Symtoms of Bladder Infection (bacterial cystitis)
- Bladder infection: Epidemiology, Symptoms and Diagnosis
- Bladder infection: treatment and prevention of acute bladder infection
Definitions
Acute cystitis is a bacterial infection of the urinary bladder, the most common manifestation of urinary tract infection (S3 German Guideline), EAU Guidelines.
- Uncomplicated bacterial cystitis: acute, sporadic or recurrent bacterial cystitis, limited to non-pregnant women with no known relevant anatomical and functional abnormalities within the urinary tract or comorbidities.
- Complicated bacterial cystitis: all urinary tract infections which are not defined as uncomplicated: in men, pregnant women, presence of anatomical or functional abnormalities, indwelling bladder catheters, renal diseases of comorbidity with risk for UTI e.g., diabetes mellitus.
Epidemiology of Bladder Infection
Prevalence of dysuria:
20–30% of adult women have an episode of dysuric symptoms one or more times a year, half of which corresponds to acute cystitis.
Prevalence of asymptomatic bacteriuria:
Below 1% in young men, 5% in healthy premenopausal women. 4–19% in old healthy patients, 15–50% in nursing home residents and up to 90% in patients with paraplegia.
Etiology (Causes) of Bladder Infection
Principles, pathogenesis and causes of UTI see section urinary tract infection.
| Erreger | % |
| Gramnegative bacteria: | |
| Escherichia coli | 77 |
| Proteus mirabilis | 5 |
| Klebsiella pneumoniae | 2–3 |
| Enterobacter spp. | 1 |
| Citrobacter spp. | < 1 |
| Other Enterobacteriaceae | 2 |
| Grampositive bacteria | |
| Staphylococcus saprophyticus | 3 |
| Staphylococcus aureus | 2 |
| Andere Staphylokokken | 4 |
| Enterococcus spp. | 3 |
| Streptococcus spp. | < 1 |
Pathology of Bacterial Cystitis
In the early stages of acute cystitis, the bladder wall shows hyperemia, edema, and infiltration by neutrophil granulocytes. In later stages, the mucosa is replaced by easily vulnerable granulation tissue. Small ulcers may develop. The lamina muscularis is usually not involved in the inflammation. Without treatment, hemorrhage and necrosis are possible.
Signs and Symptoms
- Irritable bladder symptoms: dysuria, urinary frequency, urinary urgency, and sometimes urge incontinence.
- Suprapubic pain
- Cloudy urine or hematuria
- Complication:
- Ascension of the pathogens with pyelonephritis; risk factors are vesicoureteral reflux and UTI in pregnancy.
- Emphysematous cystitis [fig. emphysematous cystitis in IVP]
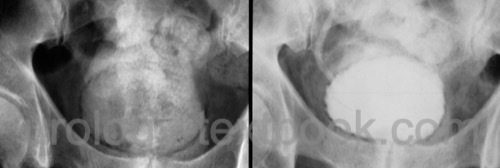 |
Diagnosis of Bladder Infection
Diagnostic Workup of Uncomplicated Cystitis in Healthy Women
Healthy women with typical symptoms of bacterial cystitis (dysuria and urinary frequency without vaginal discharge) may be treated with antibiotics with no further diagnostic workup. Urinalysis, urine culture or imaging are not absolutely necessary, since the probability for bacterial cystitis is over 70%, and the diagnostic accuracy will not improve with further workup [DGU (2009) S3-guideline for UTI].
Diagnostic Workup of Bladder Infections
Diagnostic workup of bladder infection is necessary for patients with fever, all men, patients with complicated UTI, and after failed treatment of uncomplicated cystits.
Urinalysis:
Urinalysis is performed with a dipstick or microscopic examination of the urine. Signs of a bladder infection are pyuria, bacteriuria, hematuria, or a positive nitrite test.
Urine culture:
A urine culture is recommended for complicated UTIs. 105 colony-forming units CFU/ml in a cleanly collected midstream urine indicate a UTI (Kass, 2002). A colony count from 103–104 CFU/ml may be significant in patients with typical symptoms and if typical uropathogens in pure culture (no mixed bacterial growth) are found. Forced diuresis or pollakiuria leads to a shorter retention time of the urine in the urinary bladder and can thus result in false-low bacterial counts despite UTI. Bacterial growth in a urine sample collected by catheterization or urinary bladder puncture is always pathological.
Ultrasound imaging of bladder and kidneys:
Renal ultrasound: Obstructive uropathy? Anatomical variants? Bladder ultrasound: Postvoid residual volume? Diverticula of the bladder? Bladder stones?
Vaginal examination:
Vaginal discharge should initiate a vaginal examination to diagnose vaginitis or pelvic inflammatory disease, and swabs for microbiological diagnosis are collected.
Intravenous urography:
IVU is an option in recurrent cystitis to diagnose e.g., infection stones, obstructive uropathy, diverticula or ureterocele of the bladder.
Cystoscopy:
Cystoscopy should be considered in recurrent cystitis and for differential diagnosis of hematuria (after treated acute bladder infection).
Voiding cystourethrogram:
VCUG for patients with recurrent cystitis or pyelonephritis to exclude vesicoureteral reflux, especially in children and patients with ectasia of the upper urinary tract.
Differential Diagnosis of Bladder Infection
- Vulvovaginitis
- Genital herpes
- Urethritis, gonorrhea
- Acute urethral syndrome: symptoms suggestive of bladder infection, but in the absence of significant bacteriuria
- Urinary tract infections like pyelonephritis or acute prostatitis.
- Pelvic irradiation
- Trauma: urethral irritation after sexual intercourse, after urethral manipulations, foreign body in the urinary bladder.
- Chemotherapy with cyclophosphamide
- Ketamine cystitis
- Bladder pain syndrome and interstitial cystitis
- Neurogenic lower urinary tract dysfunction
- Bladder cancer
- Psychosomatic disorder
| Bladder, diseases | Index | Bladder infection, Tx |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Bauer, H. W.; Rahlfs, V. W.; Lauener, P. A. & Blessmann, G. S. Prevention of recurrent urinary tract infections with immuno-active E. coli fractions: a meta-analysis of five placebo-controlled double-blind studies 2002, 19, 451-6.
G. Bonkat, R. Bartoletti, F. Bruyère, S. E. Geerlings, F. Wagenlehner, and B. Wullt, “EAU Guideline: Urological Infections.” [Online]. Available: https://uroweb.org/guidelines/urological-infections/
Leitlinienprogramm DGU
Interdisziplinäre S3
Leitlinie: Epidemiologie, Diagnostik, Therapie, Prävention und Management
unkomplizierter, bakterieller, ambulant erworbener Harnwegsinfektionen bei
erwachsenen Patienten. Langversion 1.1-2. AWMF Registernummer: 043/044
2017. https://www.awmf.org//uploads/tx_szleitlinien/043-044l_S3_Harnwegsinfektionen_2017-05.pdf
Fihn 2003 FIHN, S. D.:
Clinical practice. Acute uncomplicated urinary tract infection in
women.
In: N Engl J Med
349 (2003), Nr. 3, S. 259–66
Jepson, R. G.; Williams, G. & Craig, J. C.
Cranberries for preventing urinary tract infections.
Cochrane Database Syst
Rev, 2012, 10, CD001321.
Nickel 2005a NICKEL, J. C.:
Management of urinary tract infections: historical perspective and
current strategies: Part 1–Before antibiotics.
In: J Urol
173 (2005), Nr. 1, S. 21–6
Krieger 2003 KRIEGER, J. N.:
Urinary tract infections: what’s new?
In: J Urol
168 (2003), S. 2351–58.
Vahlensieck, W.; Bauer, H.-W.; Piechota, H. J.; Ludwig, M. and Wagenlehner, F. [Prophylaxis of recurrent urinary tract infections]. Urologe A, 2014, 53, 1468-1475.
 Deutsche Version: Diagnose und Therapie der akuten Zystitis
Deutsche Version: Diagnose und Therapie der akuten Zystitis
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.