You are here: Urology Textbook > Bladder > Urinary calculi
Urinary Bladder Stones – Bladder Calculi: Diagnosis and Treatment
Review literatur: (Bartosh, 2004) (Schwartz and Stoller, 2000).
Definition
Bladder stones are a common form of urolithiasis of the lower urinary tract.
Epidemiology and Causes of Bladder Stones
Endemic bladder stones:
Malnutrition in developing countries causes bladder stones in children without bladder emptying disorders. Affected areas are North Africa, the Middle and Far East. Boys under ten years suffer more often from bladder stones since girls may better pass sandy precursors via the short urethra.
The cause of urinary bladder stone formation in children is a diet mainly with cereals and too little proteins. Other factors include dehydration and a dietary phosphate deficiency. Pediatric bladder stones most commonly consist of ammonium acid urate with or without calcium, calcium oxalate, or calcium phosphate.
Secondary Bladder Stones:
Urinary bladder stones in developed countries usually form secondary due to urinary stasis, recurrent urinary tract infections, foreign bodies, or intestinal mucosa in the urinary tract (urinary diversion or augmentation).
Subvesical obstruction and bladder stones:
Postvoid residual urine (urinary stasis) is the most common cause of bladder stones (75%) and mainly affects men over 50. Benign prostatic hyperplasia or neurogenic lower urinary tract dysfunction are common causes of postvoid residual urine. Bladder stones caused by urinary stasis consist of uric acid, calcium oxalate, and magnesium ammonium phosphate (infection stone).
Urinary tract infections and catheterization:
Recurrent or chronic urinary tract infections with urease-producing bacteria lead to magnesium ammonium phosphate stones. Spinal cord injured patients with bladder catheters have a 9-fold risk for bladder stones compared to catheter-free patients with spinal cord injury. If intermittent self-catheterization or urinary condoms are necessary, the risk of bladder stones is increased 4-fold.
Foreign body:
Foreign bodies in contact with urine cause urinary stones. Self-manipulation or iatrogenic causes lead to foreign bodies in the bladder. Examples of iatrogenic causes are suture material, clips, catheters, ureteral stents, or migration of an intrauterine device.
Urinary diversion and urinary stones:
The risk of urinary stone formation (4–48%) depends on the type of urinary diversion. Urinary stones occur three times more commonly in a continent than in an incontinent urinary diversion. Risk factors are urinary stasis, mucus production, urinary tract infections, clips, non-absorbable suture material, need for catheterization, and metabolic disorders. Usually, urinary stones in urinary diversion are magnesium ammonium phosphate stones (infection stones).
Signs and Symptoms of Bladder Calculi
Childhood Symptoms in Endemic Bladder Stones:
- Abdominal pain
- Interrupted urine flow
- Dysuria, alguria, frequency
- Need to manipulate the penis
Symptoms due to Secondary Bladder Stones:
- Recurrent urinary tract infections
- Dysuria, alguria, frequency
- Interrupted urinary flow or urinary retention
- Most bladder stones cause no additional problems in addition to the underlying bladder disorder.
Complications:
Urosepsis, painful impaction in the urethra, urinary retention with postrenal kidney failure, or rarely squamous cell carcinoma of the bladder.
Diagnostic Workup of Bladder Calculi
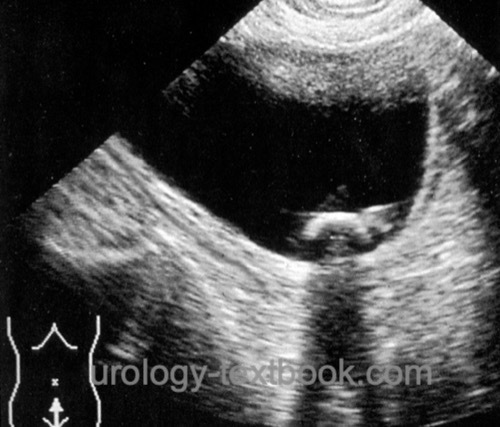
Ultrasonography:
Bladder stones imaging with ultrasonography shows an echogenic mass in the urinary bladder with posterior acoustic shadow. After repositioning, the echogenic mass should move due to gravity. Imaging is most reliable with a filled bladder.
 |
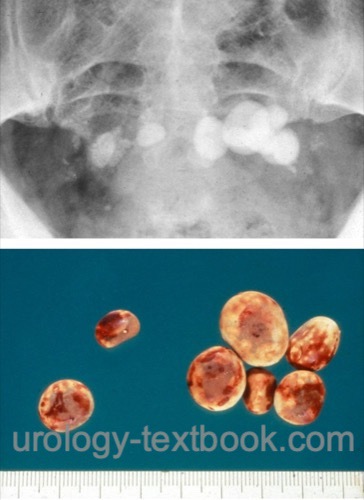
Abdominal Radiograph:
Many bladder stones are radiopaque, but some are obscured by overlying bowel gas shadows or are not radiopaque.
 |
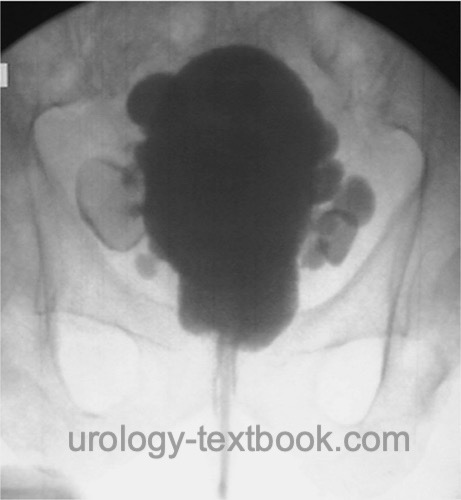
Cystography:
Non-radiopaque urinary bladder stones can be detected by cystography, causing a filling defect of the contrast medium [fig. cystography with bladder stones].
 |
Computed Tomography:
Even without contrast medium, CT scan is a reliable method for diagnosing bladder stones.
Cystoscopy:
Cystoscopy is used for diagnosing bladder stones and is also necessary for treatment planning of the underlying disease (prostate size? urethral stricture? bladder diverticula?).
Treatment of Urinary Bladder Stones
Most bladder stones are treated endoscopically. The anatomy, etiology, concomitant diseases, and stone size affect treatment options.
Extracorporeal Shock Wave Lithotripsy (ESWL):
ESWL of bladder stones is a treatment option for children or patients with a high risk for anesthesia. Without treatment of the underlying cause, there is an increased risk of recurrence.
Transurethral Cystolitholapaxy:
Mechanical or laser lithotripsy are possible options, please see technique and complications of transurethral cystolitholapaxy for details. Surgical treatment of BPH (if indicated) may be performed afterward, e.g., TURP.
Percutaneous Cystolithotomy:
Percutaneous Cystolithotomy is indicated in children or patients with large stone burden. After percutaneous puncture of the bladder and insertion of a guide wire, an access tract with 24–36 CH is established. Stone fragmentation and removal is similar to percutaneous nephrolithotomy.
Open Cystolithotomy (Sectio alta):
The decision between endoscopic or open cystolithotomy depends on the size of the stones, the number of calculi, and the size of the prostate if simultaneous surgical BPH therapy is sought. Please see the section "technique and complications of open cystolithotomy" for details.
Treatment of Endemic Bladder Stones:
After surgical removal of the bladder stones (see above), a change in diet is needed to prevent the recurrence of bladder stones: a diet rich in proteins and mixed cereals.
| Bladder diverticulum | Index | Interstitial cystitis |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Bartosh, S. M.
Medical management of pediatric stone disease.
Urol Clin North Am, 2004, 31, 575-87
Schwartz, B. F. & Stoller, M. L.
The vesical calculus.
Urol Clin North Am, 2000, 27, 333-346
 Deutsche Version: Harnblasensteine
Deutsche Version: Harnblasensteine
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.