You are here: Urology Textbook > Kidneys > Urosepsis
Urosepsis: Definition, Diagnosis, and Treatment
Definition of Urosepsis
Urosepsis is a life-threatening clinical syndrome in which complex physiological and biochemical changes to an infection of the urinary tract or male genitals lead to organ dysfunction (Singer u.a., 2016) EAU Guidelines Urological Infections
Development of Sepsis Definitions:
The understanding of sepsis is subject to constant evolution. The previous definitions of sepsis (post hoc referred to as "sepsis-1" and "sepsis-2") accounted for an excessive inflammatory response ("cytokine storm") for the pathogenesis. Recent studies confirm the importance of induced host response and organ dysfunction. This paradigm shift was essential for revising the current definition of sepsis (Weis et al., 2017).
Classic Sepsis Definition ("Sepsis-2" 2001)
Sepsis is a life-threatening systemic inflammatory response reaction (SIRS, see below) to a confirmed or suspected bacterial infection (Hotchkiss et al., 2003).
Systemic inflammatory response syndrome (SIRS):
SIRS is an inflammatory response affecting the whole organism due to significant infection or damage to the organism. SIRS is present, if two or more of the following criteria are met:
- Tachykardia: heart rate > 90/min
- Tachypnea: high respiratory rate > 20/min or
hyperventilation (pCO2 < 33 mmHg) - Fever (> 38℃) or
hypothermia (< 36℃) - Leucopenia (< 4000/μl) or
leucocytosis (> 12000/μl) or left shift with > 10% immature neutrophile granulocytes
Severe sepsis:
Severe Sepsis is the presence of sepsis criteria with at least one sign of acute organ dysfunction:
- Encephalopathy: limited vigilance, disorientation, restlessness, delirium.
- Thrombocytopenia: within 24 h, drop in platelets by more than 30% or platelet count < 100000/μl (no acute bleeding or immune system disease)
- Hypotension (systolic blood pressure < 90 mmHg or mean arterial blood pressure < 70 mmHg for at least one hour despite adequate fluid resuscitation without other causes for shock. This corresponds to the definition of septic shock.
- Hypoxia: PaO2 < 75 mmHg without explaining cardiac or pulmonary diseases
- Acute renal failure: diuresis < 0.5 ml/kgBW per hour for at least two hours despite adequate fluid resuscitation or increased serum creatinine by double the reference range
- Metabolic acidosis: BE < -5 mmol
Current Sepsis Definition ("Sepsis-3" 2017)
Sepsis is defined as a life-threatening organ dysfunction caused by an inadequate host response to an infection. Since the new definition includes organ dysfunction, every sepsis now fulfills the old term "severe sepsis" criteria. With the new definition of sepsis, a quick sepsis-related organ failure assessment score was introduced for everyday clinical practice (quick-SOFA, qSOFA) that allows early and rapid identification of patients with infections that are at increased risk of organ failure and mortality (Singer et al., 2016):
- Glasgow Coma Scale of ≤14
- Respiratory rate ≥22/min
- Hypotension with systolic arterial blood pressure < 90 mmHg
The presence of 2–3 qSOFA criteria indicates a severe course of infection with an increased risk of mortality and is a good predictor of the need for intensive care (Weis et al., 2017). A more accurate determination of the organ dysfunction and, thus, of the prognosis can be determined with the aid of the SOFA score, which is more complex and requires numerous serum parameters for the calculation.
Epidemiology of Sepsis
The incidence of severe sepsis is 3/1000. The mortality of sepsis amounts to 20%. Urosepsis has a better prognosis than other forms of sepsis, probably because of the possibility of effective causal therapy.
Etiology and Pathogenesis of Sepsis
Etiology of Urosepsis
Bacterial Infections of the Urogenital Tract:
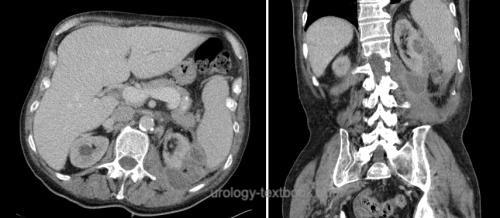
Pyelonephritis, renal abscess, infected hydronephrosis, bacterial prostatitis, epididymitis, Fournier gangrene.
Responsible bacterial organisms: E. coli, Klebsiella, Enterobacter, Serratia, Proteus, Pseudomonas, Enterococcus.
Other Causes of Sepsis (Differential Diagnosis)
Cardial infections:
Endocarditis. The bacterial spectrum is diverse: Streptococcus viridans, Enterococcus, Staphylococcus, Pseudomonas, Candida.
Respiratory infections:
Pneumonia, pleural empyema, mediastinitis, lung abscess. Bacterial spectrum: Pneumococcus, Staphylococcus, anaerobes in case of aspiration, enterobacteria, tuberculosis, Candida, Aspergillus.
Infections of the digestive tract:
Peritonitis, liver abscess, cholecystitis, cholangitis, necrotizing pancreatitis. Bacterial spectrum: E. coli, Enterobacter, Salmonella, Campylobacter, anaerobes, Enterococcus, Staphylococcus, Candida.
Infections of the ENT tract:
Tonsillitis, oral cavity floor phlegmone. Bacterial spectrum: Streptococcus pyogenes, Staph. aureus.
Infections of the CNS:
Meningococcal meningitis (sometimes with Waterhouse-Friedrichsen syndrome).
Dermal infections:
Erysipel, impetigo, dermal abscess. Bacterial spectrum: Streptococcus, Staphylococcus.
Nosocomial infections:
Catheter-associated infections (central venous catheter, bladder catheter), implants, wound infection, pneumonia. Diverse bacterial spectrum.
Pathogenesis of Urosepsis
Immune system response:
Patients with sepsis present with an initial excessive immune response, followed by immunosuppression. Causes for the transition from hyperinflammation to immunosuppression are the depletion of proinflammatory cytokines, lymphocyte apoptosis, and the formation of anergy. Several genetic risk factors that influence the immune system are known, which increase the case fatality rate of sepsis.
Hyperinflammation:
The presence of the bacteria induces an excessive immune response, which causes significant damage to the host organism. Although the responsible cytokines are partially known (TNF-α, interleukin 1 and 2, interferon-γ), clinical trials to block these cytokines have failed to improve the prognosis of sepsis.
Immunosuppression:
The following signs indicate immunosuppression: lack of delayed hypersensitivity reaction, limited ability to remove the infection and predisposition to nosocomial infections. Immunosuppression is associated with decreased secretion of proinflammatory cytokines in response to bacterial antigens (see below). Furthermore, anti-inflammatory cytokines are increasing (e.g., interleukin 4 and 10). The stimulation of the immune reaction with interferon-γ may lead to an improvement of the prognosis. Sepsis can begin immediately in this immunosuppressive state, this correlates with reduced symptoms (no fever) and a poor prognosis.
Cellular mechanisms of organ dysfunction:
Autopsy studies failed to identify microscopic changes in kidney, myocardial, or liver cells that could explain pronounced organ dysfunction with mortality. Cell dysfunction ("cell stunning or cell hibernating") is explained by the influence of the cytokines and metabolites of sepsis, which disturb the body cell's mitochondrial function and energy production. The following metabolic shutdown and organ dysfunction can largely recover after the survival of sepsis.
Signs and Symptoms of Urosepsis
Local symptoms:
Local symptoms depend on the underlying disease causing urosepsis (see above).
General symptoms of urosepsis:
Fever, chills, hyperventilation, tachycardia, and hypotension are the classic symptoms. Hypothermia indicates a poor prognosis. Furthermore, altered mental status, somnolence, oliguria, or anuria.
Diagnosis of Urosepsis
Vital signs:
Heart rate, blood pressure, respiratory rate, urine output, and vigilance are essential for assessing the prognosis and initiating intensive care measures.
Urine culture:
Collect urine culture before starting calculated antibiotic treatment, e.g., when inserting a bladder catheter, ureteral splint, or nephrostomy.
Blood cultures:
Collect blood cultures before starting calculated antibiotic treatment.
Further microbiological diagnosis:
Before starting a calculated antibiotic, depending on the suspected infection: sputum, stool, wound secretions, cerebrospinal fluid.
Laboratory tests:
Blood count, coagulation tests with AT III and fibrinogen, CRP, liver parameters, creatinine, blood gas analysis, procalcitonin as a marker for sepsis.
Imaging in Urosepsis:
Ultrasound of the urogenital organs, abdominal CT scan, and chest X-ray depending on the clinical situation.
Treatment of Urosepsis
Treatment of urosepsis is an emergency and requires immediate intensive care, empiric intravenous antibiotic treatment, and evaluation for a causal therapy.
Intensive Care Therapy:
Quick administration of oxygen and intravenous fluids to normalize blood pressure and oxygen saturation is essential for a good prognosis.
Oxygen and Fluid Management:
Begin with 30 ml/kg of fluid in adults in the first three hours. The aim is to create a balance between oxygen consumption and oxygen transport within six hours, shown by the normalization of central venous oxygen saturation, lactate concentration, base excess (BE), pH, and urine output.
Vasopressor therapy:
If fluids are insufficient to achieve a mean arterial blood pressure over 65 mmHg, administering vasoactive and positive inotropic substances such as noradrenaline or adrenaline is necessary.
Treatment of organ failure:
Mechanical ventilation and renal replacement procedures (hemofiltration) are often necessary.
Antibiotic treatment:
After obtaining blood cultures and cultures from other sites (see above), empiric intravenous antibiotic therapy should be started within one hour after diagnosis of sepsis: e.g., Amoxicillin/clavulanic acid combined with gentamicin, 3rd generation cephalosporins or reserve antibiotics such as imipenem or meropenem (depending on suspected resistance or severity of sepsis). Anaerobic infections are possible with peritonitis, wound infections, or Fournier gangrene and may require additional use of metronidazole. Antibiotic therapy is necessary for at least 7–14 days, depending on the clinical course.
Causal Treatment of Urosepsis
Numerous diseases causing urosepsis can be improved by surgical means. Depending on the cause, consider appropriate diagnostics in order not to overlook surgical options:
- Pyelonephritis: drain renal/pararenal abscesses, nephrectomy of a nonfunctioning kidney.
- Hydronephrosis: retrograde ureteral splint or percutaneous nephrostomy.
- Prostatitis: suprapubic catheter, drainage of abscesses.
- Fournier gangrene: radical excision of the necroses.
- Epididymitis: drain abscess and orchiectomy
| Urinary tract infections | Index | Surgical site infections |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
G. Bonkat, R. Bartoletti, F. Bruyère, S. E. Geerlings, F. Wagenlehner, and B. Wullt, “EAU Guideline: Urological Infections.” [Online]. Available: https://uroweb.org/guidelines/urological-infections/
Hotchkiss und Karl 2003 HOTCHKISS, R. S. ; KARL,
I. E.:
The pathophysiology and treatment of sepsis.
In: N Engl J Med
348 (2003), Nr. 2, S. 138–50
Singer, M.; Deutschman, C. S.; Seymour, C. W.;
Shankar-Hari, M.; Annane, D.; Bauer, M.; Bellomo, R.; Bernard, G. R.;
Chiche, J.-D.; Coopersmith, C. M.; Hotchkiss, R. S.; Levy, M. M.;
Marshall, J. C.; Martin, G. S.; Opal, S. M.; Rubenfeld, G. D.; van der
Poll, T.; Vincent, J.-L. & Angus, D. C.
The Third International
Consensus Definitions for Sepsis and Septic Shock (Sepsis-3).
JAMA, 2016,
315, 801-810
 Deutsche Version: Definition und Ursachen der Urosepsis
Deutsche Version: Definition und Ursachen der Urosepsis
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.