You are here: Urology Textbook > Bladder > Stress urinary incontinence in women > symptoms and diagnostic workup
Stress Urinary Incontinence in Women
- Stress urinary incontinence in women: definition and etiology
- Stress urinary incontinence: symptoms and diagnostic workup
- Stress urinary incontinence: medical and surgical treatment
Signs and Symptoms of Stress Urinary Incontinence
According to the classification of Stamey, there are three grades of clinical SUI:
- Grade 1: loss of urine with a relevant increase in abdominal pressure, e.g., coughing, sneezing, or laughing.
- Grade 2: loss of urine with a lesser increase of abdominal pressure, e.g., walking or standing up.
- Grade 3: loss of urine unrelated to physical activity or position, e.g., standing or lying in bed.
Other symptoms: pelvic organ prolapse, urge symptoms (frequency, nocturia), residual urine or urinary retention, and recurrent urinary tract infections.
Diagnostic Workup
History:
Ask for micturition symptoms, incontinence severity (pad usage), degree of bother, previous surgery, number of vaginal deliveries, medications (e.g., alpha-blocker, clonidine), and neurological and urological diseases. Ask for pelvic organ prolapse symptoms, e.g., bowel symptoms and symptoms of sexual dysfunction.
Urine analysis:
Urine sediment and urine culture to exclude a urinary tract infection.
Quantification of Stress Urinary Incontinence:
Documentation of drinking quantities, micturition volumes, incontinence episodes and pad changes with a micturition diary helps to quantify urinary incontinence. A time period of 24 to 48 hours is usually sufficient. For motivated patients with digital scales at home, the severity of the incontinence can be determined by weighing the incontinence pads each change.
Pad test for quantification of SUI:
An alternative to weighing the pads by the patient during the micturition protocol: a weighted pad is used after filling the bladder to 50% of its capacity. The patient should perform defined provocation exercises (stair climbing, jumping, coughing), and the pad should be weighed again. Urine loss of more than 25 g is considered severe urinary incontinence.
Physical Exam:
In addition to a neurological examination, a vaginal and rectal examination is done in the lithotomy position. Significant pathological findings are cystocele or rectocele, quantification of the pelvic floor insufficiency, anal sphincter tone and anal reflex, clitoral or bulbocavernous reflex, provocation of incontinence with pressure, coughing, or heel impact test.
Q-tip test:
A sterile, lubricated cotton or dacron swab is inserted into the urethra just until the end of the urethra/beginning of the trigonum of the bladder. The patient performs a Valsalva provocation. If the angle of the Q-tip rotates more than 30 degrees, a urethrovesical hypermobility is probable.
Marshall-Bonney test:
The Marshall-Bonney test tries to anticipate the clinical effect of a suspension operation: the paraurethral tissue is lifted with the index and middle fingers, and the patient is asked for coughing or Valsalva provocation with a full bladder.
Ultrasound Imaging:
- Bladder sonography: to measure residual urine, bladder wall thickness or reveal bladder anomalies.
- Vaginal or perineal ultrasound: can demonstrate the bladder neck opening under Valsalva provocation, a significant risk factor for stress incontinence.
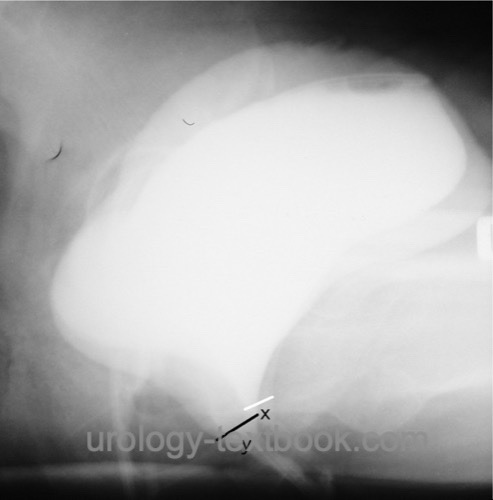
Voiding Cystourethrography:
Voiding cystourethrography (VCUG) is often done in combination with urodynamics to diagnose cystocele, hypermobile urethra, rotation of the urethra, opening of the bladder neck under stress, and to exclude other forms of incontinence (extraurethral incontinence) [VCUG performed for stress urinary incontinence].
 |
Urodynamic Examination:
Urodynamic is the gold standard for diagnosing the cause of urinary incontinence. Urodynamics can be dispensed with if stress urinary incontinence is undoubtful without further symptoms. A urodynamic measurement should be done in patients with mixed urinary incontinence, reduced urinary bladder capacity, postvoid residual volume, or pronounced pelvic floor insufficiency.
The primary task of urodynamics is less the detection of SUI than the exclusion of complicating concomitant diseases that endanger the success of surgery. The demonstration of SUI can be achieved by a urethral pressure profile and by measurement of the Valsalva leak point pressure (VLPP). It is sometimes impossible to prove SUI with urodynamic testing due to the presence of the measurement catheter. The Valsalva leak point pressure (VLPP) measurement may also be performed without the catheter, and the abdominal pressure is detected with the rectal probe.
Valsalva leak point pressure (VLPP): a Valsalva maneuver is performed until urine leakage and the intra-abdominal and intravesical pressures are measured.
Cystoscopy:
Cystoscopy is indicated to assess bladder capacity and sphincter function, and for differential diagnosis. Specific signs of stress urinary incontinence do not exist.
Defecography or dynamic magnetic resonance imaging of the pelvic floor:
Defecography or MRI imaging of the pelvic floor may reliably image cystocele, rectocele, enterocele, or prolapse under stress. The pubococcygeal line is often specified as a reference point.
| Stress incontinence | Index | SUI treatment |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Dean, N. M.; Ellis, G.; Wilson, P. D. & Herbison, G. P. Laparoscopic colposuspension for urinary incontinence in women.Cochrane Database Syst Rev, 2006, 3, CD002239
Gilling, P. J.; Wilson, L. C.; Westenberg, A. M.; McAllister, W. J.; Kennett, K. M.; Frampton, C. M.; Bell, D. F.; Wrigley, P. M. & Fraundorfer, M. R. A double-blind randomized controlled trial of electromagnetic stimulation of the pelvic floor vs sham therapy in the treatment of women with stress urinary incontinence.
BJU Int, 2009, 103, 1386-1390
Latthe, P. M.; Singh, P.; Foon, R. & Toozs-Hobson, P. Two routes of transobturator tape procedures in stress urinary incontinence: a meta-analysis with direct and indirect comparison of randomized trials.
BJU Int, 2010, 106, 68-76
Liedl u.a. 2005 LIEDL, B. ; SCHORSCH, I. ; STIEF, C.: [The development of concepts of female (in)continence. Pathophysiology, diagnostics and surgical therapy].
In: Urologe A
44 (2005), Nr. 7, S. W803–18; quiz W819–20
Petros, P. E. & Ulmsten, U. I.
An integral
theory of female urinary incontinence. Experimental and clinical
considerations.
Acta Obstet Gynecol Scand Suppl, 1990,
153, 7-31.
Quek, P.
A critical review on magnetic stimulation:
what is its role in the management of pelvic floor disorders?
Curr
Opin Urol, 2005, 15, 231-235
Ward, K. L.; Hilton, P.; K., U. & Group, I. T. T.
Tension-free
vaginal tape versus colposuspension for primary urodynamic stress
incontinence: 5-year follow up.
BJOG, 2008, 115,
226-233
Viktrup u.a. 2004 VIKTRUP, L. ; SUMMERS,
K. H. ; DENNETT, S. L.:
Clinical practice guidelines for the initial management of urinary
incontinence in women: a European-focused review.
In: BJU Int
94 Suppl 1 (2004), S. 14–22
 Deutsche Version: Klassifikation und Diagnose der Stressinkontinenz
Deutsche Version: Klassifikation und Diagnose der Stressinkontinenz
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.