You are here: Urology Textbook > Anatomy > Urinary bladder
Gross Anatomy of the Urinary Bladder: Trigone, Blood Supply, and Sphincter
References: (Benninghoff, 1993).
Surface Anatomy of the Bladder
The bladder is ovoid and has a volume capacity of 400–500 ml. The bladder can be divided into the corpus with two lateral walls, the dorsal wall and the ventral wall. The dorsal and ventral walls meet at the apex, and the urachus starts and runs to the umbilicus. The bladder neck surrounds the bladder trigone (see below).
Adjacent organs of the urinary bladder
The bladder lies preperitoneal behind the symphysis; the peritoneum covers parts of the ventral and dorsal walls. The space anterior to the bladder and behind the abdominal wall is called retropubic space (space of Retzius). The space enables various filling conditions of the urinary bladder. The bladder is adjacent to the small intestine and sigmoid colon (dorsal, towards the abdomen). The iliac vessels are lateral to the bladder. The bladder neck in men contacts the prostate. In women, the bladder trigone and bladder neck are cranial to the vagina, and the uterus is located posterior to the bladder.
Peritoneum and Anatomy of the Inner Surface of the Abdominal Wall
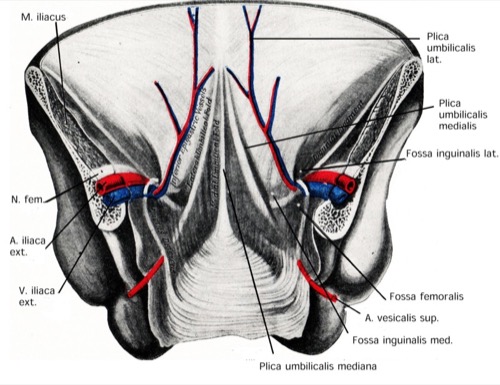
The peritoneum covers the rectum and the dorsal wall of the bladder, forming a peritoneal pouch in the pelvis: rectovesical pouch in men (excavatio rectovesicalis), and recto-uterine pouch in women (excavatio vesicouterina). The urinary bladder and adjacent structures determine the inner surface of the lower abdominal wall [fig. anatomy of the inner surface of the abdominal wall]:
- median umbilical fold (urachus)
- medial umbilical fold (obliterated umbilical artery)
- lateral umbilical fold (inferior epigastric vessels)
 |
Interior of the Bladder
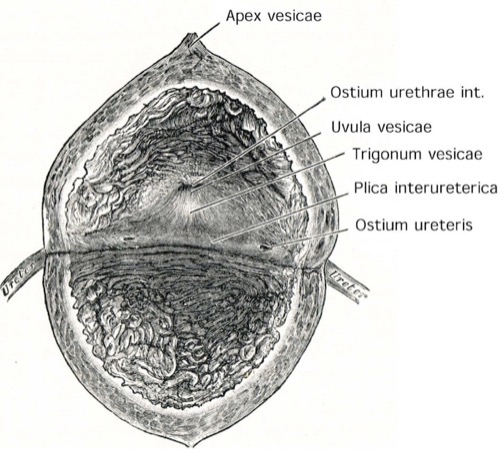
The interior areas of the bladder are the trigone of the bladder (trigonum vesicae), side walls, rear and front walls [fig. interior of the bladder].
 |
Trigone of the bladder
The internal urethral orifice (Ostium urethrae internum) and both orifices of the ureters (ostium ureteris right and left) limit the trigone of the bladder. The plica interureterica is a mucosa fold between the orifices of the ureters and helps to identify the orifices during transurethral ureteral catheterization. The wall of the bladder trigone consists of three layers:
Ureter and the superficial bladder trigone:
The ureter enters obliquely through the bladder wall. The inner smooth muscle layer of the ureter forms with the inner smooth muscle layer of the contralateral ureter the superficial trigone. The superficial trigone extends into the prostatic urethra to the seminal colliculus in men and to the external urethral orifice in women. Thus, the superficial bladder trigone is a tubular structure above the orifices of the ureter and flat below the orifices.
Waldeyer Sheath and the deep trigone bladder:
A separate external smooth muscle layer (Waldeyer Sheat) accompanies the distal ureter to the bladder. After passing through the bladder wall, the Waldeyer Sheath forms with fibers of the detrusor muscle the deep trigone of the bladder. Like above, these muscle fibers range from two orifices of the ureter to the bladder neck.
Detrusor muscle of the bladder:
The inner longitudinal layer extends into the urethra in women until the ostium urethrae externum, and in males until the caudal end of the prostate. The middle circularly arranged layer and the outer longitudinal layer extend to the bladder neck. In women, they surround the urethra and support the external urinary sphincter. The detrusor muscle is innervated by parasympathetic nerve fibers (S2–4).
Uretero-vesical valve:
The contraction of the trigone pulls the orifices of the ureters caudal to the bladder neck. This results in a substantial increase in uretero-vesical resistance. The dysfunction of the trigone (transection, lumbar sympathectomy) may lead to vesicoureteral reflux. Second, the contraction of the trigone reduces the resistance of the bladder neck, thus facilitating urination. Third, the rise of vesical pressure during bladder filling and voiding also compresses the ureters due to the oblique passage through the bladder wall and is an essential element for valve function.
Sphincter of the Urinary Bladder
The sphincter of the urinary bladder consists of smooth muscle (internal sphincter muscle) and striated muscle (external sphincter muscle).
Internal sphincter muscle:
The smooth muscle of the bladder trigone surrounds longitudinally as well as circularly the bladder neck (see above).
External sphincter muscle:
The striated external sphincter muscle has a horseshoe-shaped aspect. In women, he surrounds the middle and proximal urethra. In men, the muscle surrounds the entire length of the membranous urethra. In both cases, the striated sphincter has close contact with the pelvic floor muscles.
Anatomy of the female urethra
Please refer to Section: Anatomy of the female urethra.
Vascular supply of the Bladder
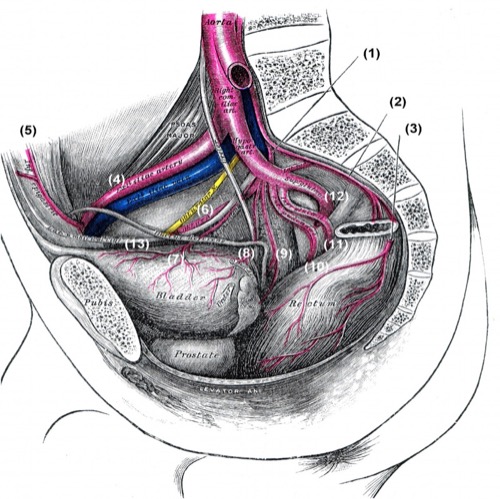
Branches of the internal iliac artery: A. iliolumbalis (1), A. sacralis mediana (2), A. rectalis media of the contralateral side (3), A. iliaca externa (4), A. epigastrica inferior (5), A. obturatoria (6), A. vesicalis superior (7), A. vesicalis inferior (8), A. rectalis media (9), A. pudenda interna (10), A. glutea inferior (11), A. glutea superior (12), A. umbilicalis und Lig. umbilicale (13). Fig. from Gray’s Anatomy, Lea and Febiger 1918, Philadelphia, USA.
Arteries of the bladder
- Superior vesical artery: from the non-obliterated portion of the umbilical artery
- Inferior vesical artery: directly from the internal iliac artery.
- Smaller branches: from the uterine artery in women, obturator artery, and internal pudendal artery.
Veins of the bladder:
The blood from the bladder drains into the vesical venous plexus. The internal iliac vein receives the blood from the vesical venous plexus.
Lymphatic Vessels:
The lymphatic drainage of the bladder involves the external iliac, internal iliac, obturator, and sacral lymph nodes. From there, lymph passes via the common iliac lymph nodes to the paracaval and paraaortic lymph nodes.
Innervation of the bladder
Somatic nervous system:
The pudendal nerve from the sacral plexus controls the striated external sphincter muscle. Afferent nerve fibers of the pudendal nerve measure the urinary bladder filling (via the stretch of the urothelium) and the contraction of the detrusor muscle (via the wall tension).
Autonomic nervous system:
Parasympathetic preganglionic neurons are located in the sacral cord (S2 to S4) and run via the ventral roots to the parasympathetic ganglia next to the pelvic organs. In the case of the bladder, the ganglions are located in the detrusor muscle and the vesical venous plexus.
The preganglionic sympathetic nerve fibers come from the thoracolumbar cord (TH1 to L2) and are switched to postganglionic fibers in the ganglia of the sympathetic trunk. The postganglionic fibers run via the hypogastric nerve into the pelvis.
The innervation of the detrusor muscle is mainly parasympathetic. While the sympathetic innervation of the detrusor muscle is of secondary importance, the bladder neck is innervated by the sympathetic nervous system to close the bladder neck during ejaculation. The parasympathetic, sympathetic, and somatic nervous systems have afferent nerve fibers, which pass through the dorsal root to the spinal cord.
| Anatomy | Index | Bladder Histology |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Benninghoff, A. (1993): Makroskopische Anatomie, Embryologie und Histologie des Menschen. 15. Auflage. München; Wien; Baltimore: Urban & Schwarzenberg.
 Deutsche Version: Anatomie der Harnblase
Deutsche Version: Anatomie der Harnblase
Urology-Textbook.com – Choose the Ad-Free, Professional Resource
This website is designed for physicians and medical professionals. It presents diseases of the genital organs through detailed text and images. Some content may not be suitable for children or sensitive readers. Many illustrations are available exclusively to Steady members. Are you a physician and interested in supporting this project? Join Steady to unlock full access to all images and enjoy an ad-free experience. Try it free for 7 days—no obligation.
New release: The first edition of the Urology Textbook as an e-book—ideal for offline reading and quick reference. With over 1300 pages and hundreds of illustrations, it’s the perfect companion for residents and medical students. After your 7-day trial has ended, you will receive a download link for your exclusive e-book.