You are here: Urology Textbook > Anatomy > Pelvic cavity
Anatomy of the Pelvic Cavity
Muscles of the Pelvic Floor
The pelvic floor muscles may be separeted into the pelvic diaphragm, urogenital diaphragm and superficial perineal muscle layer. Fibers of all three layers have contact (are inserting) at the perineal body (central tendon of perineum).
Pelvic Diaphragm
The pelvic floor muscle consists of the levator ani and coccygeus muscle.
Levator Ani:
Funnel-shaped flat pelvic floor muscle originating from the symphysis and fascia obturatoria (parts are called tendinous arc). The muscle fibers of both sides pass downward and backward to the middle line of the pelvic floor, where they meet their contralateral counterpart to form the levator sling, which surrounds the rectum. Ventral to the rectum remains a muscle gap of the levator ani, through which the urogenital organs pass [Fig. pelvic floor muscles].
Coccygeus Muscle
The coccygeus muscle is located dorsally to the levator ani. Origin: sacrospinous ligament and ischial spine. Insertion: coccyx.
Urogenital Diaphragm
The urogenital diaphragm is located caudal to the pelvic diaphragm and closes the ventral gap of the levator ani. The urogenital organs pass through this flat muscle plate. The muscles of the urogenital diaphragm are the external urethral sphincter, superficial and deep transverse perineal muscles [Fig. pelvic floor muscles]. The urogenital diaphragm is surrounded by fascias: the perineal membrane (inferior layer) and superior fascia of the urogenital diaphragm.
Superficial Perineal Muscles of the Pelvic Floor
External Anal Sphincter
The external anal sphincter surrounds circularly the anus and measures about 8–10 cm in length.
Bulbospongiosus Muscle
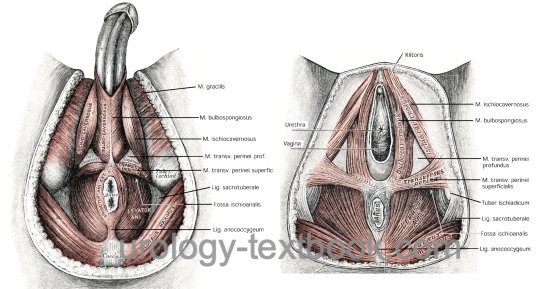
The bulbospongiosus muscle is a superficial perineal muscle covering the bulb of the penis (in men) and surrounding the vestibulum (in women). The external anal sphincter and the bulbospongiosus muscle form a figure-eight-shaped muscle loop, especially in women, with the central tendon of the perineum in the middle.
Ischiocavernosus Muscle
The ischiocavernous muscle is a superficial perineal muscle covering the crus of the penis (in men) or the crus of the clitoris (in women). In the female the vestibular vaginae is surrounded. The muscle fibers run from ischium to the corpus cavernosum of the penis or clitoris [Fig. pelvic floor muscles].
 |
Arteries of the Pelvic Cavity
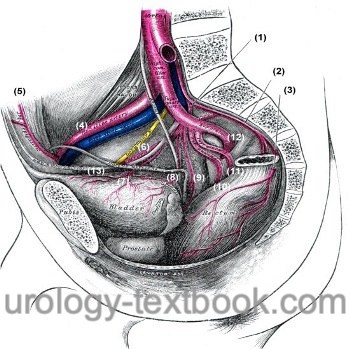
Arteries of the pelvic cavity: A. iliolumbalis (1), A. sacralis mediana (2), A. rectalis media der Gegenseite (3), A. iliaca externa (4), A. epigastrica inferior (5), A. obturatoria (6), A. vesicalis superior (7), A. vesicalis inferior (8), A. rectalis media (9), A. pudenda interna (10), A. glutealis inferior (11), A. glutealis superior (12), A. umbilicalis und Lig. umbilicale (13). Fig. modified from Gray’s Anatomy, Lea and Febinger 1918, Philadelphia, USA.
The common iliac artery divides after a short distance into the external iliac and internal iliac artery [Fig. arteries of the pelvic cavity].
Parietal Branches of the Internal Iliac Artery
The parietal branches supply the wall of the pelvis cavity and reach structures outside of the pelvic cavity through bone and muscle gaps.
- Iliolumbar artery (latin: A. iliolumbalis) (1)
- Lateral sacral artery (latin: A. sacralis lateralis)
- Obturator artery (latin: A. obturatoria) (6): passes through the canalis obturatorius into the adductor muscles. Before that, a strong anastomosis to the inferior epigastric artery rarely arises (corona mortis).
- Superior gluteal artery (latin: A. glutealis superior) (12): passes through the suprapiriform foramen into the gluteal muscles.
- Inferior gluteal artery (latin: A. glutealis inferior) (11): passes through the infrapiriform foramen into the gluteal muscles and thigh.
Visceral Branches of the Internal Iliac Artery
- Umbilical artery (latin: A. umbilicalis) (13): branches of the superior vesical artery (7).
- Inferior vesical artery (latin: A. vesicalis inferior) (8)
- Uterine Artery (latin: A. uterina) in woman
- Middle rectal artery (latin: A. rectalis media) (9)
- Internal pudenda artery (latin: A. pudenda interna) (10): passes through the foramen infrapiriformis into the fossa ischiorectalis. In a fascial duplication of the obturator fascia (Alcock's canal), the artery (together with nerve and vein) runs to the anus and external genitals. Branches of the internal pudendal artery: the inferior rectal artery (A. rectalis inf.), perineal artery (A. perinealis), bulbourethral artery (A. bulbi penis), deep artery of the penis (A. profunda penis), dorsal artery of the penis (A. dorsalis penis).
Branches of the External Iliac Artery
Shortly before the entering the lacuna vasorum (then named femoral artery), the following branches are released:
- Inferior epigastric artery (A. epigastrica inferior) (5): with branches: cremasteric artery and possibly an anastomosis with the obturator artery (named corona mortis).
- Deep circumflex iliac artery (A. circumflexa iliaca profunda)
Veins of the Pelvic Cavity
The veins of the pelvis cavity follow above mentioned arteries and drain into the internal iliac veins. The common iliac vein is formed by the internal and external iliac veins. The confluence of the left and right common iliac vein at the level of the fifth lumbar vertebra gives rise to the inferior vena cava.
Lymphatic Drainage from the Pelvic Cavity
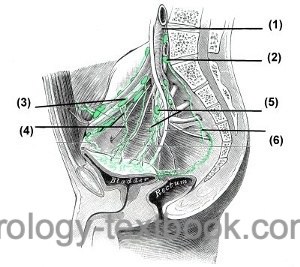
The lymphatic vessels largely follow the course of the veins. Lymph node groups exist as: external iliac lymph nodes, internal iliac lymph nodes, common iliac lymph nodes, obturator lymph nodes, pararectal and sacral lymph nodes. The pelvic lymph nodes drain into the lumbar lymph nodes and reach via the left and right lumbar lymph trunk the cysterna chyli [Fig. pelvic lymph nodes].
 |
| Abdominal cavity: veins | Index | Groin anatomy |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Benninghoff 1993 BENNINGHOFF, A.: Makroskopische Anatomie, Embryologie und Histologie des Menschen.15. Auflage.
München; Wien; Baltimore : Urban und Schwarzenberg, 1993
 Deutsche Version: Anatomie der Beckenhöhle
Deutsche Version: Anatomie der Beckenhöhle