You are here: Urology Textbook > Surgery (procedures) > Prostate biopsy
Prostate Biopsy
Indications for Prostate Biopsy
Prostate biopsy is indicated in cases of suspected prostate cancer:
- Increased or rising PSA concentration
- Suspicious digital-rectal examination
- Suspicious imaging of the prostate gland
Technique of Prostate Biopsy
Patient Preparation
- Discontinuation of anticoagulant agents (aspirin, warfarin, ticlopidine ...)
- Exclusion or treatment of a urinary tract infection
- Perioperative antibiotic prophylaxis.
Anesthesia for Prostate Biopsy
Periprostatic infiltration anesthesia with local anesthetic, preferably in combination with a diclofenac suppository. 10–20 ml of local anesthetic is infiltrated on both sides of the prostate in the region of the neurovascular bundles before the biopsy. Additional infiltration of the skin and needle path through the pelvic floor is necessary for transperineal biopsy. For prostate biopsies with high number of samples, a spinal or general anesthesia is useful.
Prostate Biopsy
Prostate biopsy is performed with either a transrectal or transperineal technique. Prostate cores are gained with a 18G true cut biopsy needle under transrectal ultrasound imaging control.
Number and location of the prostate samples:
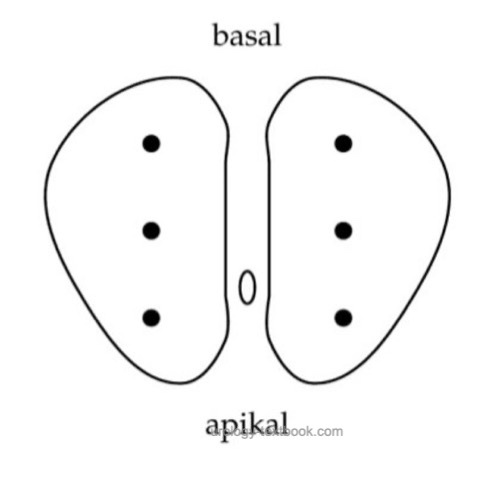
The minimum of prostate samples are six cores (sextant biopsy), three from each prostate lobe (apical, middle and basal) [sextant prostate biopsy] (Hodge et al., 1989). The EAU guidelines on prostate cancer recommend at least 10 biopsy cores [Heidenreich (Eur Urol 2008)].
 |
Suspicious (hypoechoic) lesions of the prostate should be biopsied in addition. This increases the likelihood of prostate cancer detection. The prostate cores are sent separately to the pathologist, this enables later conclusions for e.g., nerve sparing radical prostatectomy.
Biopsing the prostate in the region of the prostate capsule, sextant prostate biopsy can detect more cancers (Stamey, 1995). The biopsy needle advances 2 cm into the tissue, this must be anticipated before biopsy. Especially apical biopsies can injure the dorsal venous plexus of the prostate.
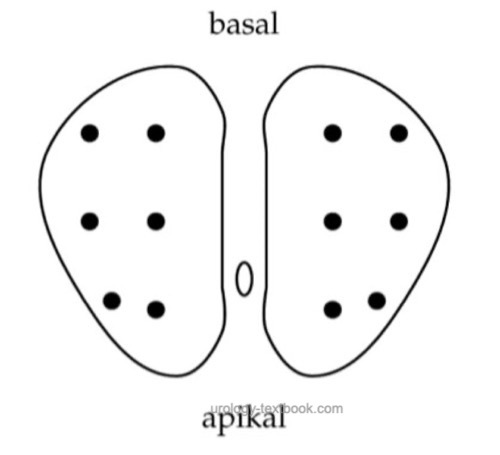
Prospective studies demonstrated an improved sensitivity by increasing the prostate core number. The additional sampling should be obtained near the organ capsule of the prostate and from the transitional zone [fig increased sampling in prostate biopsy]. Not all randomized trials have demonstrated this effect. Additionally, increased sampling may detect more clinically insignificant prostate cancers.
80% of prostate cancers are diagnosed with the first prostate biopsy, 10% with the second prostate biopsy, 7% with the third prostate biopsy and 3% with the fourth prostate biopsy.
 |
Complications of Prostate Biopsy
Mild complications are relatively common (over 50%), serious complications are uncommon (Rodriguez and Terris, 1998).
Infections after prostate biopsy:
Acute prostatitis. Rare infectious complications are sepsis (1%), there are reports about fatal sepsis due to anaerobic bacteria.
Bleeding:
50% of patients have minor hematuria for up to seven days. Hematospermia in 30%, this can last up to a month. Severe rectal bleeding can be managed with rectal packing or endoscopic coagulation.
Other complications of prostate biopsy:
- Urinary retention (1–2%)
- Vasovagal reaction (5%)
- Adverse reactions from the local anesthetic, such as dizziness, nausea, syncope, cardiac arrhythmias or seizures.
| Urologic Surgery | Index | TURP |
Index: 1–9 A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
References
Hodge u.a. 1989 HODGE, K. K. ; MCNEAL, J. E. ; TERRIS, M. K. ; STAMEY, T. A.: Random systematic versus directed ultrasound guided transrectal core biopsies of the prostate.In: J Urol
142 (1989), Nr. 1, S. 71–4; discussion 74–5
Rodriguez und Terris 1998 RODRIGUEZ, L. V. ;
TERRIS, M. K.:
Risks and complications of transrectal ultrasound guided prostate
needle biopsy: a prospective study and review of the literature.
In: J Urol
160 (1998), Nr. 6 Pt 1, S. 2115–20
Stamey 1995 STAMEY, T. A.:
Making the most out of six systematic sextant biopsies.
In: Urology
45 (1995), Nr. 1, S. 2–12
 Deutsche Version: Prostatabiopsie
Deutsche Version: Prostatabiopsie